Home » CLL / SLL Patient Education Toolkit » What is Bone Marrow?
What is Bone Marrow?
In science and medicine, information is constantly changing and may become out-of-date as new data emerge. All articles and interviews are informational only, should never be considered medical advice, and should never be acted on without review with your health care team.
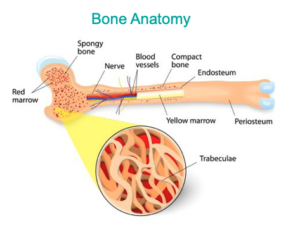 Bone marrow is where we make nearly all of our blood, so it is obviously vitally important. It has been estimated that the bone marrow makes more than 220 billion new red blood cells daily. About 1% of the body’s total red blood cells are replaced every day.
Bone marrow is where we make nearly all of our blood, so it is obviously vitally important. It has been estimated that the bone marrow makes more than 220 billion new red blood cells daily. About 1% of the body’s total red blood cells are replaced every day.
It is a busy factory that is always open to make all the cellular blood components. When it is healthy and has all the necessary raw material such as iron, folate and vitamin B12, it can quickly respond to increased demands such as producing more white cells when needed to fight infections or red cells when we are anemic or platelets when we are bleeding.
If our bone marrow is damaged by radiation or chemotherapy or if most of the normal bone marrow healthy cells are crowded out or suppressed by cancer, then our prospects can be grim. Bone marrow failure can be a dire situation.
That is why our motto has always been to protect your bone marrow and your immunity when choosing a therapy for CLL or for any cancer.
Takeaway Points
- The bone marrow makes nearly all of our cellular blood.
- It makes up about 4% of our total body.
- When it is not functioning, we cannot make red cells, white cells or platelets.
- When healthy, it is responsive and flexible to the changing demands from the rest of the body.
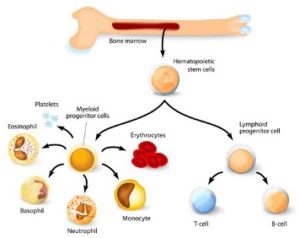
- The marrow is full of primitive blood stem cells that make many different types of mature cells.
- The red marrow that makes the blood comprises about half the marrow in adults, but can expand if needed.
- The yellow marrow supports the red marrow and makes various connective tissues.
 Structure:
Structure:
Bone marrow is a soft, jelly-like tissue that fills the centers of bones known as the medullary cavities.
It is protected by the hard outer layer of bone known as the periosteum.
This is the bone that must be pierced in a bone marrow biopsy or aspirated to get to the marrow needed for assessment. There are two types of bone marrow: red and yellow.
Red bone marrow:
Red bone marrow or myeloid tissue consists of a highly vascular, fibrous tissue containing the hematopoietic or blood forming stem cells.
White blood cells last anywhere from a few hours to a few days, platelets for about 10 days, and red blood cells for about 120 days. These cells must be constantly replaced by the bone marrow.
For example, the process of a developing and releasing a mature red cell into the blood stream from its bone marrow precursor takes about 7 days.
Yellow bone marrow:
Yellow bone marrow is more fatty and contains mesenchymal stem cells or marrow stromal (connective tissue) cells. These are stem cells that produce mature fat, cartilage, muscle and bone cells.
Bone marrow stem cells
Stem cells are primitive cells that have the capacity to turn into a number of different types of cell.
Test on the bone marrow:
Bone marrow aspiration uses a hollow needle to remove about 1 ml of liquid bone marrow which can then be examined under a microscope. The needle is usually inserted into the hip or occasionally sternum in adults. A bone marrow biopsy uses a different type of needle that removes a solid core of bone tissue that is fixed and thinly sliced to be examined. The two tests are usually done together.
Summary:
Our bone marrow is a remarkably flexible and resilient organ that performs many functions, mostly as the factory for our blood and connective tissue. With a healthy bone marrow, we can respond successfully against many of the dangerous health challenges we face with CLL. When it is damaged by disease or therapy, we are at a distinct disadvantage.

