Some see CLL / SLL as a solved problem. But unfortunately, we know better. This abstract from the European Hematology Association (EHA) Annual Congress in 2022 reinforced one of our greatest unsolved problems: what happens following treatment with a covalent BTK and BCL2 inhibitor.
This is sometimes called double refractory or double exposed and is one of the areas CLL Society is actively promoting research.
Covalently (irreversibly) binding Bruton’s tyrosine kinase inhibitors (cBTKi) such as ibrutinib and acalabrutinib and the only approved B-cell lymphoma 2 inhibitor (BCL2i), venetoclax, have revolutionized the care and significantly improved outcomes for patients with CLL / SLL. These agents work amazingly well, but they are palliative, and eventually, most patients will need to be treated again.
This trial sought to expand our limited data when patients are seen in these two classes of drugs by reviewing real-world data in a large electronic medical database for those with CLL / SLL between December 2011 and October 2020.
Results:
- 339 patients (median age 66 years, male 69.6%) met eligibility criteria. Please note that this was a respective review. We know that these patients had been exposed to both classes of drugs.
- Of these 339, 215 could be evaluated who had stopped both.
- The authors do not share details as to why they stopped, such as progression or intolerance or reaching remission though Richter’s transformation was recorded among 24 (7.1%).
- 47 patients (21.9% of the 215 who discontinued therapy) died before receiving subsequent therapy
- 116/215 (54%) received subsequent therapy
- 52/215 (24.2%) were alive without additional treatment after cBTKi/BCL2i
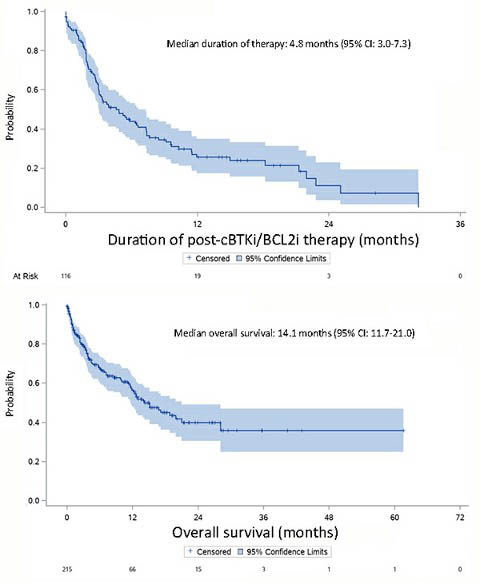
- The median time from discontinuation of cBTKi/BCL2i (whichever agent was last) to the immediate following treatment discontinuation, transformation, or death was only 4.6 months.
- Among those who received subsequent therapy, the most common immediate next line of therapy included additional BCL2i-based therapy (venetoclax re-treatment with or without other agents, n=71/116; 61.2%) or anti-CD20 antibody-based therapy (with or without other agents, 73/116 (62.9%).
- Fewer patients received PI3K inhibitor-based treatment (n=14/116; 12.1%) or additional cBTKi therapy (n=19/116; 16.4%).
- The median duration of the next therapy for those who were “double exposed” was less than five months.
- Worse, among the 215 who discontinued cBTKi/BCL2i therapy, the median overall survival (OS) was only 14.1 months.
Conclusion:
Double exposed patients with CLL / SLL don’t do well, as proved by these rather grim statistics on time to next treatment discontinuation, duration of the subsequent therapy, and overall survival. The authors conclude, and we wholeheartedly agree: “There remains a need for more effective therapies for patients with CLL / SLL after progression on cBTKi/BCL2i“.
Watch my monologue on the abstract below:
The actual EHA abstract is Outcomes Following Treatment With a Covalent BTK and BCL2 Inhibitor Among Patients With Chronic Lymphocytic Leukemia (CLL)/Small Lymphocytic Lymphoma (SLL): A Real-World Study of a Large U.S. Database.
Less mature data were presented at the American Society of Hematology Annual Meeting in 2021: Addressing a New Challenge in Chronic Lymphocytic Leukemia: Outcomes of Therapies after Exposure to Both a Covalent Bruton’s Tyrosine Kinase Inhibitor and Venetoclax.
We still have much work ahead of us, but with new molecules and synergistic combinations being developed and trialed, there are reasons for optimism.
Stay strong. We are all in this together.
Brian
Brian Koffman MDCM (retired) MS Ed (he, him, his)
Co-Founder, Executive VP, and Chief Medical Officer CLL Society, Inc.

