Reviewed by Dr. Brian Koffman
The Bottom Line:
Access to healthcare may be a significant contributor to racial and ethnic disparities in survival outcomes for patients with blood cancers such as chronic lymphocytic leukemia (CLL). While minority groups experienced worse outcomes than White patients in the general U.S. healthcare system, there were no survival differences between racial / ethnic groups in the Veterans Affairs healthcare system, which lacks barriers to access.
Who Performed the Research and Where Was it Presented:
Dr. Rockbum Kim and colleagues from Baylor College of Medicine presented the results at the American Society for Hematology (ASH) Annual Meeting 2023.
Background:
It is well-documented that there are racial disparities in cancer incidence and outcomes, with Black patients having the highest mortality rate for most leading cancer types. People of color may be at increased risk of developing certain cancers due to environmental exposures and / or genetic factors. Social and economic inequities can create barriers to accessing health care, which in turn limit access to cancer screening, care, and treatment. Discrimination and bias within the healthcare system may also contribute to disparities in care and outcomes. This study examined survival outcomes in patients with different types of blood cancers across different healthcare settings.
Methods and Participants:
This study used data from electronic cancer registries representing three different healthcare systems to identify adult patients with newly diagnosed lymphoma, myeloma, or leukemia from 2011 to 2020. For each patient cohort, researchers assessed the impact of race / ethnicity on overall survival.
The three different data sets were:
- Surveillance, Epidemiology, and End Results Program (SEER) is a program that provides national cancer statistics for the U.S. It covers 22 U.S. geographic areas, and its demographics represent the U.S. population.
- Veterans Affairs (V.A.) national healthcare system – a unique single-payer system with patients covered by veteran benefits.
- Harris Health System (HHS) – an extensive county hospital system in the Houston metropolitan area where a large proportion of patients are uninsured and receive charity care.
Results:
- The demographics of the three patient cohorts are shown in the table below.
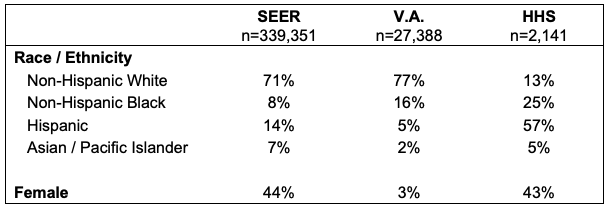
- SEER patients were more representative of the U.S. census, while the vast majority of V.A. patients were male (97%).
- Both V.A. and HHS had higher proportions of non-Hispanic Black patients.
- In the SEER cohort, minority groups had an increased risk of death compared with non-Hispanic Whites across all cancer types (lymphoma, leukemia, myeloma).
- In the V.A. cohort, survival was similar or better for minority groups compared with non-Hispanic Whites across all cancer types.
- In the HHS cohort, there were no significant differences in survival between minority groups and non-Hispanic whites, except non-Hispanic Blacks had a higher risk of death from lymphoma compared with non-Hispanic Whites.
Conclusions:
As seen in the SEER cohort, racial / ethnic disparities in survival outcomes for patients with blood cancers continue to persist in the U.S. population. Interestingly, minority status was neutral or even protective in the V.A. system, which does not have barriers to access. However, minority status was associated with worse outcomes in the HHS system, where many patients experience barriers to access due to a lack of insurance. This suggests that access to healthcare may be a significant contributor to racial / ethnic disparities in survival outcomes for patients with blood cancers.
Links and Resources:
The ASH abstract is Racial / Ethnic Disparity for Hematologic Malignancies in Different Healthcare Systems in the U.S.
Take care of yourself first.
Ann Liu, PhD
